What is Acute Cholecystitis?
Acute cholecystitis refers to a sudden inflammation of the gallbladder, usually triggered by an infection. In most cases, this occurs when a gallstone blocks the duct that drains bile from the gallbladder, leading to a buildup of pressure, irritation, and eventually infection. In some instances, long-standing inflammation of the gallbladder can gradually worsen and develop into an acute infectious condition.
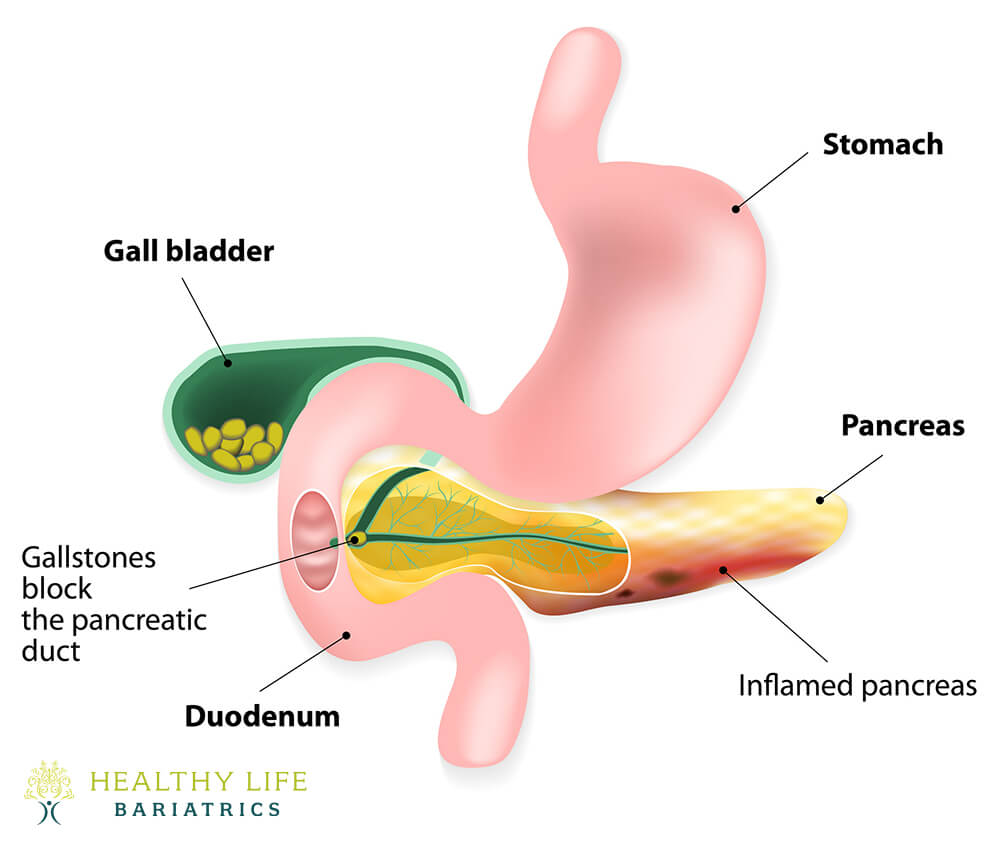
Table of Contents
- What is Acute Cholecystitis?
- Symptoms of Acute Cholecystitis
- Acute Cholecystitis Causes
- Risk Factors for Acute Gallbladder Inflammation
- Acute Cholecystitis Diagnosis Testing
- Acute Cholecystitis Disease Progression Risks
- General Approaches Treating Acute Inflammation and Infection
- Acute Cholecystitis Treatment
- Recovery After Acute Cholecystitis Surgery
- Specialized Acute Cholecystitis Care by Dr. Babak Moein in Los Angeles, CA
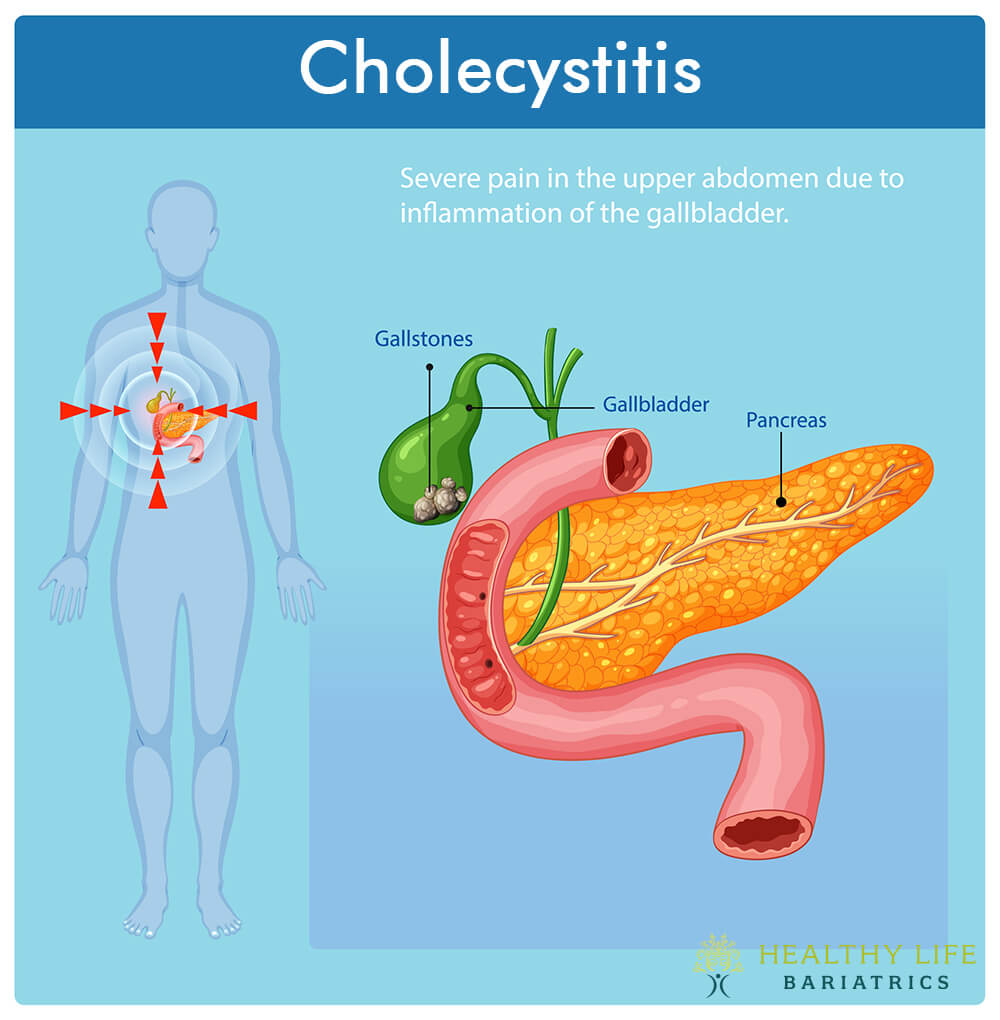
Symptoms of Acute Cholecystitis
Acute cholecystitis often occurs in patients with a history of biliary colic. Its pain typically starts in the upper abdomen and spreads to the right side under the ribs. Unlike the sharp, fluctuating pain of biliary colic, this pain is steadier and milder. A key diagnostic sign is Murphy's sign pain upon deep inhalation during palpation of the right upper abdomen.
Other common symptoms include nausea, vomiting, and a persistent fever that doesn’t respond well to medications like paracetamol. These symptoms tend to worsen after large or fatty meals. If left untreated, the fever can become more intense and continuous over time.
Acute Cholecystitis Causes
There are two possible causes for this potentially severe condition. We can group those causes into two categories:
1. Calculous Cholecystitis
Calculous cholecystitis is the most common category of acute cholecystitis, accounting for most cases. This condition occurs when a gallstone blocks the gallbladder opening (cystic duct). Biliary sludge can also contribute to duct blockage.
Biliary sludge combines bile and tiny crystals composed of salt and cholesterol. The duct blockage occurs when bile builds up inside the gallbladder. Too much bile increases the pressure inside the organ, leading to inflammation. For one out of five patients, the gallbladder becomes affected by a bacterial infection.
2-Acalculous Cholecystitis
Acalculous cholecystitis is a form of gallbladder inflammation that occurs without gallstones, often due to reduced bile flow. Acalculous cholecystitis is more prevalent among those who are severely ill, recovering from severe surgery or trauma, and those with compromised immune systems.
It commonly results in pain in the upper-right portion of the abdomen. It has the potential of speeding up in case appropriate medical care is not sought. If appropriate care is not obtained in time, this condition may lead to serious complications like infection with pus in the gallbladder (empyema), tissue death(gangrene), or even gallbladder rupture. It is normally treated with IV antibiotics and in most instances requires surgical removal of the gall bladder.
Risk Factors for Acute Gallbladder Inflammation
- Known causative agents for acute cholecystitis are:
Pre-existing Gallstones – Impactions result in inflammation of the gall bladder mucosa
Obesity - Further makes immobile stone expulsions difficult. - Infection: Local or systemic extension from the gallbladder or bile contents.
- High Estrogen – It influences the bile composition and gallbladder motility disorders in women.
Metabolic Syndrome. - Type 2 diabetes and Dyslipidemia are associated with Metabolic Syndrome.
- FAMILY HISTORY - More than half have family members with gallstones who ultimately required cholecystectomies.
- Though it can occur in anyone, early diagnosis and treatment can help to prevent its worsening or emergency situations in high-risk patients.
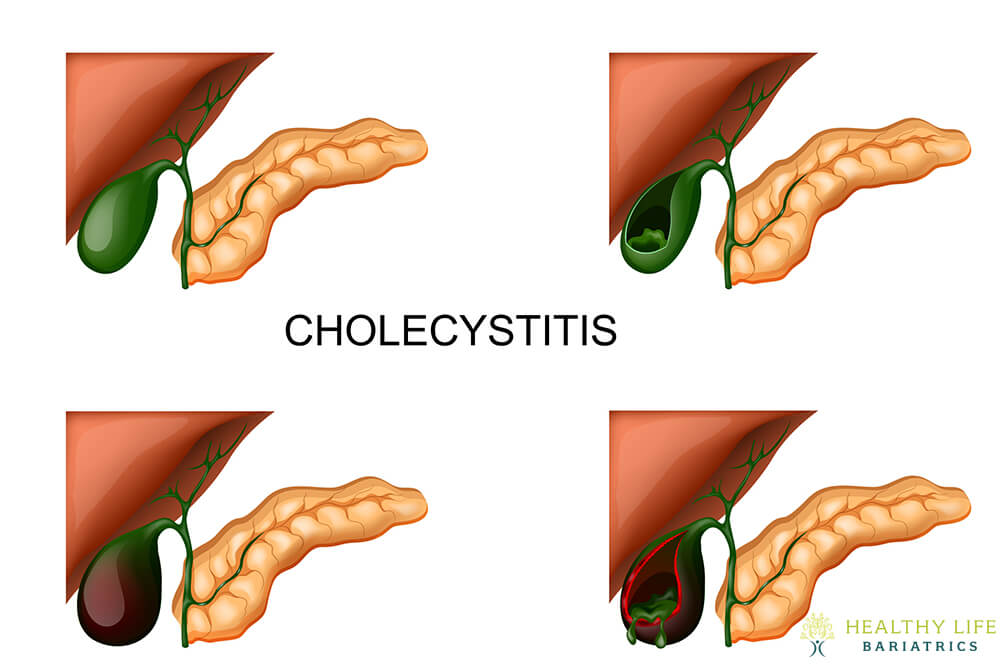
Acute Cholecystitis Disease Progression Risks
Gallbladder inflammation often passes within a few days if the obstruction clears spontaneously, allowing bile drainage to resume. However, persistent blockages risk severe septic progression, tissue death, and structural compromises, mandating emergency surgery in up to 20% of hospitalized patients. Rare grave outcomes like gallbladder rupture spilling infected bile throughout the abdomen necessitate rapid open-operative interventions if necrosis and abscess formation develop unchecked by antibiotics.
General Approaches Treating Acute Inflammation and Infection
Most patients hospitalized with acute cholecystitis improve within 72 hours of supportive medical treatment aimed at:
- Pain Management: Patient-controlled IV analgesia and regional anesthetic blocks relieve discomfort to the greatest degree prior to the resolution of fever when both oral and other routes can be used.
- Intravenous Fluids/Electrolyte Administration: Vomiting and abdominal losses make replenification necessary.
- Bowel Rest/Nutrition: The patient's diet is increased to a clear liquid diet once the nausea lessens. Bowel rest in terms of avoiding ingestion due to the presence of.
- Antibiotics: Broad-spectrum gram-negative/anaerobic agents have proven effective in greater than 85% of infections. Culture-directed narrow-spectrum antimicrobials are continued if bacteriuria
- Cholecystostomy Tubes: Placement by means of radiologic guidance, percutaneous techniques in obstructed gall bladders immediately relieve shelf stones obstructing gall bladder outlets in critically ill patients who are not stable for emergent surgery.
Currently, acute cholecystitis receives urgent and targeted treatment based on contemporary medical standards suited to every patient’s specific circumstances. At Healthy Life Bariatrics, with its experienced team led by Dr. Babak Moeinolmolki, patients receive appropriate care focusing on their safety and best possible outcomes regarding treatment, it be through current state-of-the-art medical protocols.
Acute Cholecystitis Treatment
There have been some changes in the management of acute cholecystitis in Los Angeles from delayed open cholecostectomy to early laparoscopic cholecystectomy within 1 to 5 days, resulting in reduced complications, shorter mean hospital stays, and lower total costs.
Current options for the procedure include:
Early Laparoscopic Surgery: This is recommended for more stable patients and is an effective way of preventing further breakdowns.
Delayed Surgery - It is conducted only on high-risk patients having multiple medical issues, to enable complete stabilization of the patient before the removal of the gallbladder.
Recovery After Acute Cholecystitis Surgery
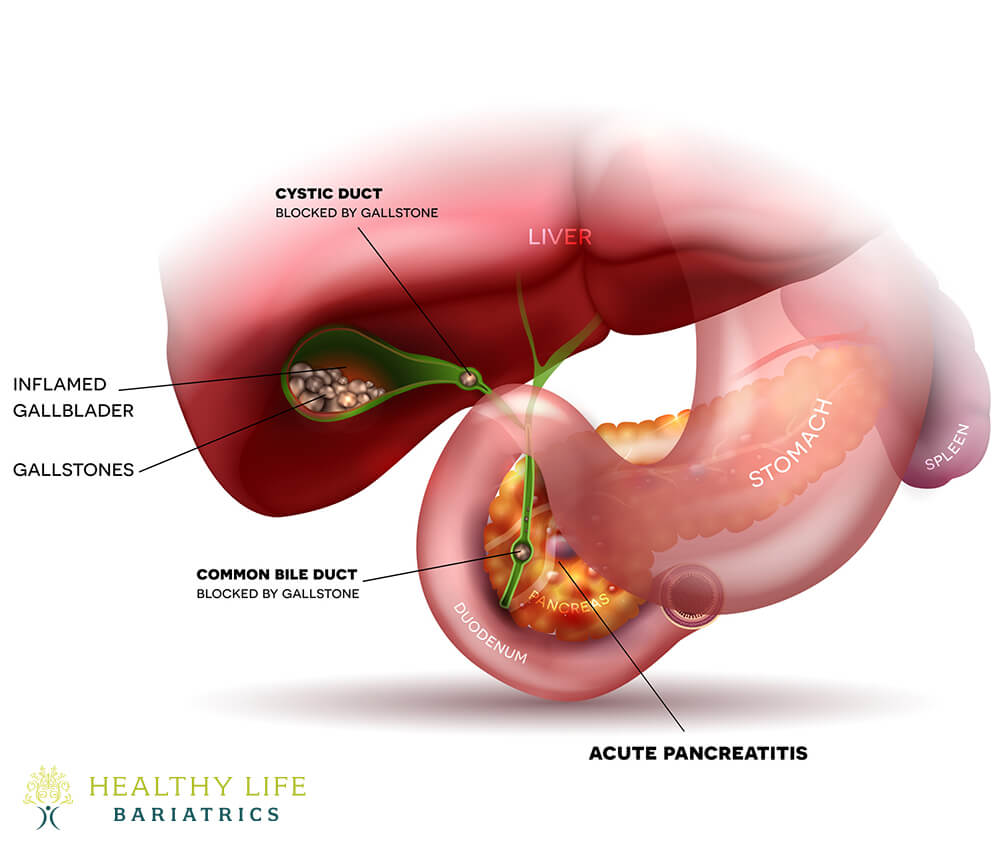
In most cases, after early laparoscopic surgery of the gallbladder, the patient can recover quickly. In the first week, the patient can just take oral medication for pain, eat normally, and perform light exercise. By the second week, most of the swelling and discomfort will have faded away, and the patient can drive a car, go back to office work, and perform light exercise. In the succeeding months, there is gradual improvement in energy, and sustained relief is attained, with more than 95% improvement in symptoms. In those requiring surgery, although recovery is extended because of delayed surgery, it is still effective.
Specialized Acute Cholecystitis Care by Dr. Babak Moein in Los Angeles, CA
Diagnosing an ailment like acute cholecystitis is essential as soon as possible. A consultation with world-class general surgeon Dr. Babak Moein can provide you with a diagnosis for the condition, and peace of mind. Get your questions answered and feel relieved that surgery for your acute gallbladder inflammation is only a short time away. Call Healthy Life Bariatrics to book your meeting with Dr. Moein from anywhere you are in Los Angeles, California. (310)861-4093.
Find Out More:


